Case Report | DOI: https://doi.org/10.31579/2835-8295/158
Management of Chronic Morbidities of Elimination of Lymphatic Filariasis
*Corresponding Author: Suresh Kishanrao, Family Physician & Public Health Consultant, Bengaluru.
Citation: Suresh. K, (2026), Management of Chronic Morbidities of Elimination of Lymphatic Filariasis, International Journal of Clinical Reports and Studies, 5(2); DOI:10.31579/2835-8295/158
Copyright: © 2026, Suresh. K. This is an open-access artic le distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: 24 February 2026 | Accepted: 30 March 2026 | Published: 15 April 2026
Keywords: filarial elephantiasis; hydrocoele; parasitic worms; wuchereria bancrofti; brugia malayi; brugia timori; mosquito vectors (culex, anopheles, aedes); mass drug administration; triple combination therapy; elimination of lymphatic filariasis
Abstract
Lymphatic filariasis is a parasitic infection caused by 3 species of parasitic worms namely Wuchereria Bancrofti, Brugia Malayi, Brugia Timori, transmitted by Culex, Anopheles, and Aedes mosquitoes. It causes chronic, irreversible lymphatic damage, leading to severe swelling of legs known as elephantiasis or of the scrotum known as hydrocele. Lymphatic filariasis impairs the lymphatic system and can lead to the abnormal enlargement of body parts, causing pain, severe disability and social stigma. Recent involvement in the management of a Filarial elephantiasis of both limbs leading to restricted movements, this article is intended to explain the developments in the management of Filarial elephantiasis from simple personal hygiene to current practice of Pneumatic pressure among cases not suitable for surgical debridement. While Global Mass Drug Administration (MDA) has significantly reduced the prevalence by two thirds from 199 million cases in 2000, to 66 million people, (a 74% decline) and 23 countries have been validated by the WHO as having eliminated LF as a public health problem, as of 2025, approximately 657 million people in 39 countries remain at risk of Lymphatic Filariasis (LF) and require preventive chemotherapy. Morbidity Management of Chronic Cases involves i) rigorous washing of affected areas with soap and water, combined with antiseptic creams, to prevent secondary bacterial infections, ii) elevation of limbs and, iii) wearing compression garments to reduce swelling. In extreme swelling cases surgery is performed to remove damaged tissue or treat hydroceles. Off late Elephantiasis of legs is managed using air pressure massager or compressor for cases which are not fit for surgery.
Materials & Methods: This article is the outcome of a recent learning about managing a severely swollen bilateral elephantiasis in an elderly lady, through Pneumatic pressure application for a case not fit for surgical debridement. Authors autobiography and his brother’s story Filarial hydroceles through surgical intervention 5 decades ago and multiple moderately swollen cases through triple drug therapy, elevation of limbs and compression through elastic crape bandages or wearing compression garments add to the discussions Outcome: The elderly lady is benefited in reducing the swelling and able to move around herself achieving about 40% reduction in the bilateral swellings of the limbs.
Introduction
Filarial Elephantiasis or lymphatic filariasis is a parasitic infection caused by 3 species of parasitic worms namely Wuchereria Bancrofti, Brugia Malayi, Brugia Timori, transmitted by Culex, Anopheles, and Aedes mosquitoes. It causes chronic, irreversible lymphatic damage, leading to severe swelling of legs known as elephantiasis or the scrotum – ‘Hydrocele’. Lymphatic filariasis impairs the lymphatic system and can lead to the abnormal enlargement of body parts, causing pain, severe disability restricting mobility and social stigma [1,2]. It commonly occurs between 30-45 years of age and a little more commonly in males than in females, it is usually unilateral; but rarely bilateral with one limb in higher grade than other as was in our case. Clinically lymphoedema is classified into 4 stages [3,4].
As of 2025, approximately 657 million people in 39 countries remain at risk of Lymphatic Filariasis (LF) and require preventive chemotherapy. While Global Mass Drug Administration (MDA) has significantly reduced the prevalence by two thirds from 199 million cases in 2000, to 66 million people, who suffer from chronic manifestations like lymphedema & hydrocele. As of 2025, 66 million people were infected a 74?cline since the start of WHO’s Global Programme to Eliminate Lymphatic Filariasis in 2000. As of late 2025, 23 countries have been validated by the WHO as having eliminated LF as a public health problem. Eliminating lymphatic filariasis (LF) as a public health problem is defined as - ‘Reducing the infection rate to a level where it no longer poses a major health burden meaning “microfilaria rate is less than 1% in the sentinel population and children born after the initiation of mass drug administration are free from circulating antigenemia”. Due to successful implementation of strategies, 871 million people no longer require preventive chemotherapy [9].
Management focuses on mass drug administration (MDA), a large-scale distribution of combinations s ivermectin + diethylcarbamazine (DEC) + albendazole for transmission control and hygiene-based care for morbidity. An Individual Treatment is done using Diethylcarbamazine (DEC) which kill microfilariae and some adult worms. Antibiotics – Doxycycline is used to kill Wolbachia, an endosymbiotic bacteria necessary for the worm's survival, which can help reduce swelling. Albendazole/Ivermectin: used in conjunction with other drugs to kill parasites. Using insecticide-treated mosquito nets, spraying, and reducing mosquito breeding sites are some of the preventive methods [8,9].
Morbidity Management of Chronic Cases involves i) rigorous washing of affected areas with soap and water, combined with antiseptic creams, to prevent secondary bacterial infections, ii) elevation of limbs and, iii) wearing compression garments to reduce swelling. In extreme swelling cases surgery is performed to remove damaged tissue or treat hydroceles. Off late Elephantiasis of legs is managed using air pressure massager or compressor for cases which are not fit for surgery [8],
This article is based on managing one such Bilateral Filarial bilateral limb elephantiasis justifying Pneumatic compressor use than surgical debridement and lessons learnt
Case Reports:
1 Kalavathy -Bilateral Elephantiasis Legs:
Ms Kalavathi aged about 75 years, a retired Government Primary school teacher from Raichur in Karnataka is suffering from Filarial Elephantiasis grade III since late 1990’s and Stage IV since last 2 years. The district is one of the Filariasis endemic districts in Karnataka. She was admitted to a private tertiary care hospital in Bengaluru with heavy swelling and inability to walk since a fortnight under a plastic surgeon’s care. Though not life threatening it had incapacitated her for over last 30 years. The history revealed that it started first in the right leg when she was around 16 years old and slowly spread from toes to thighs. After 2 years even the left leg got affected.
She is also having Vitiligo or Leukoderma from early childhood, and both conditions have left her unmarried. Leukoderma is the loss of skin colour (whitening of skin). leukoderma developed in the setting of pre-existing idiopathic vitiligo, suggesting a genetic predisposition. This genetic susceptibility idiopathic in many though in some Liver and thyroid disease have been reported and some others getting leukoderma upon contact with certain chemicals. However, her case there is neither a personal nor family history of vitiligo nor another autoimmune disease.
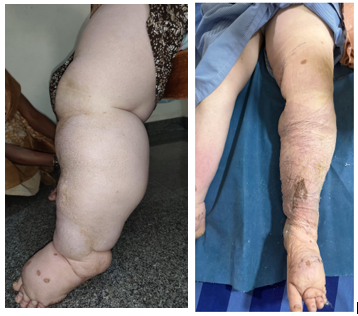
Left Leg on admission 8 Jan 2026 Left Leg after a week of Crape elastic Bandaging 15 Jan 2026
After a thorough examination a general surgeon and the plastic surgeon tried Crape elastic bandage for a week. On this authors intervention both opined that surgical debridement at her age is risky and either the bandaging or even better is to use Pneumatic Pressure technique. After discussions a Pneumatic pressure, specifically in the form of Intermittent Pneumatic Compression (IPC) or Sequential Intermittent Pneumatic Compression (SIPC) was considered best option. SIPC equipment was bought costing INR 35,000.
She and one attendant were trained to use the same in the hospital for a week before discharge, after about 3 weeks use there is reduction of swelling in both limbs by about 40%. Further development is being monitored.
Case of Filarial Hydrocoele:
This author and his elder brother are two live examples of affected by Filarial Hydrocoele in early adulthood.
Case 1. autobiography
: The author got his left sided hydrocelectomy done in 1969 at the age of 20 years. Known as Lords procedure it involved plication of the sac. After administering spinal anaesthesia, a small incision was made in the scrotum and accessed the fluid-filled sac. The accumulated fluid was drained via suction. The scrotal incision was closed with absorbable sutures. This technique is preferred for small-medium sized hydroceles with a thin sac, has a reduced risk of haematoma when compared to Jaboulay procedure. The right sided surgery in 1995 by when the technique had changed to Jaboulay procedure in which the sac is opened drained, partially excised, everted and sutured behind the testicle. Despite being a greater risk of haematoma this author recovered without many consequences.
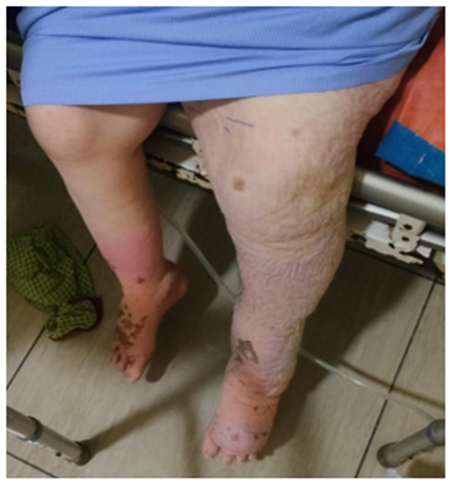
Results after use of Pneumatic Compressor for 3 weeks
Case 2: The author’s elder brother went through the first type of surgery (Lords) bilaterally in 1972. He suffered infertility .The causes of Infertility Post-Hydrocelectomy may be i) A large, untreated hydrocele can act as a heat-retaining layer, raising the scrotal temperature above the required level for healthy spermatogenesis ii) Large, long-standing hydroceles exerts sustained pressure on the testicle, causing tissue shrinkage & damage iii) A post-operative infection or pre-existing chronic inflammation could reduce sperm production iv) Increased pressure can potentially compromise blood supply to the testicle.
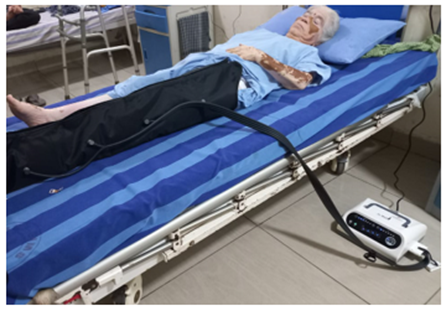
Pneumatic Compressor training
Discussions:
Filarial lymphatic oedema is a chronic, irreversible lymphatic damage, leading to severe swelling of legs known as elephantiasis or the scrotum ‘Hydrocele’. Lymphatic filariasis impairs the lymphatic system and can lead to the abnormal enlargement of body parts, causing pain, severe disability and social stigma [1,2].
Pathology of Elephantiasis: Filarial Elephantiasis involves foot and leg only. Mild lymphoedema may extend into the thigh but there is no distinct line of demarcation between the healthy and diseased skin. The sole of the foot escapes because of the firm attachment of the skin with the planter fascia; and partly be due to weight-bearing. All the elephantoid process occurs outside the deep fascial envelope, the deeper tissues being normal, probably due to entry of infective larvae into the superficial lymphatic system of the limb following the mosquito-bite. The limb is swollen to a variable degree with thick and rough skin. Near the ankle, many grooves may develop, due to the movements of the ankle, which become deeper as the disease advances. Later, the skin may develop many nodular excrescences on the toes and foot. The skin cuts like an unripe pear and the subcutaneous tissue shows a blubbery appearance, with a lot of watery fluid exuding out from dilated spaces and lymphatics. The adipose tissue is replaced by fibrous tissue. The vascularity of the tissues is increased, especially the Venous components. Microscopically, there is excessive deposition of fibrous tissue, which is maximum in the der-mis, and becomes less towards the deeper plane. This phenomenon was described as "Chronic inflammatory fibromatosis of hypertrophy or the hypodermal & dermal connective tissue “by Matas (1913). The eIephantoid tissue is infiltrated by eosinophils, plasma cells and monocytes with giant cells around dead or calcified worms. Increased number of mast cells have also been found. The lymphatics show obliterative end a-lymphangitis with scarring [3].
Epidemiology & Clinical Features: It commonly occurs between 30-45 years of age and a little more commonly in males than in females, it is usually unilateral; but rarely bilateral with one limb in higher garde than other as was in our case. As the disease develops through a series of events, clinically lymphoedema is classified: Stage I The patient has recurrent attacks of filarial fever with lymphangitis leading to pitting oedema of the limb, usually reversible on elevation of the affected limb. Stage II. '''With subsidence of attack; the swelling reduces but the "status quo ante" is seldom attained. Mostly non-pitting oedema, which does not reverse on elevation. Skin changes may begin to appear. Stage III: With subsequent attacks there is further increase in lymphoedema, every attack adding to the swelling and severe skin changes like dermatosclerosis (thickening) & papillomatous lesions Stage IV: The skin becomes rough. dry, thickened with loss of elasticity. It cannot be pinched or moved on deeper tissue, and the hairs become sparse [3,4].
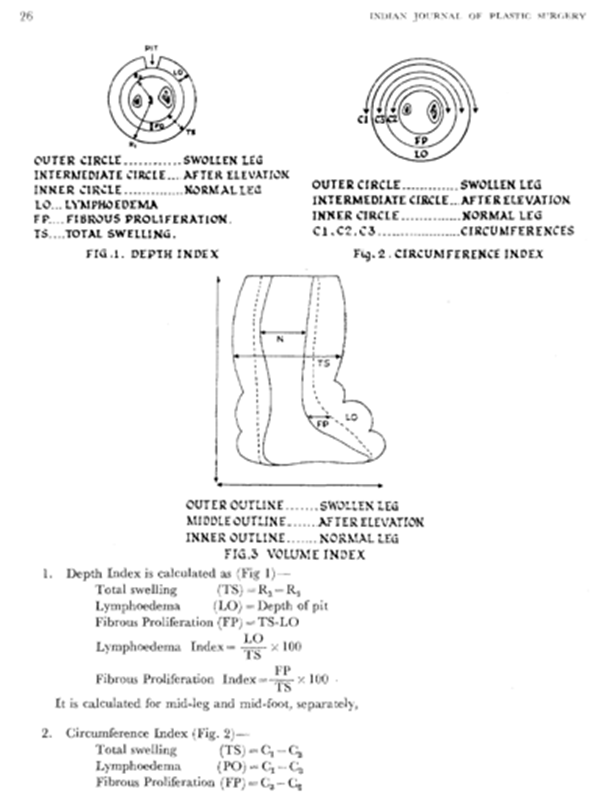
In a study of lymphoedema caused due to bancroftian filariasis by objective assessment of movement of joints and power of muscles in the affected legs, a total of 81 consecutive lymphoedema patients attending a filariasis clinic in Pondicherry urban locality indicated that Of the cases assessed, 40% in grade-I, 55% in grade-II, 77.3% in grade-III and 94.7% in grade-IV lymphoedema cases had functional limitations either in joint movements or power of muscles or both. The effective loss of locomotor/function (combined loss of joint movement and power of muscles in %) increased with stage of lymphoedema (grade-I-4.3+7.4, grade-II-7.0+8.4, grade-III-15.4+14.8 and grade IV- 33.2+22.8) [3]
As of 2025, out of approximately 657 million people in 39 countries at risk of Lymphatic Filariasis (LF) Africa, is estimated to have over 22 million cases of clinical manifestations with 16.3 (80%) million men having hydrocele. Predicted total disease burden in Africa for 2025 is 2.2 million Disability-Adjusted Life Years (DALYs) lost. Similarly, Lymphatic Filariasis (LF) remains a significant public health challenge in India, with about 650 million people at risk across 339 endemic districts in 2025 which accounts to about 60?ses of the global burden, with reported cases 620,000 suffering from lymphedema and over 150,000 from hydrocele. The government aims to eliminate LF by 2027 [9,10]. Given the current situation it is unlikely to achieve this goal.
Management of Lymphatic Filarial (LF) limbs in India is shifting from just morbidity control to active, community-based elimination by 2027. Key trends include the triple-drug therapy (IDA: Ivermectin, DEC, Albendazole), rigorous Morbidity Management and Disability Prevention (MMDP) for lymphedema, and improved surveillance. The focus is on early diagnosis using antigen tests & reducing acute ADLA episodes to improve quality of life [10].

Individual Case Management: Crepe bandaging: For the management of filarial elephantiasis (filarial lymphedema) in India especially in public sector and for patients who can’t spend money on buying pneumatic Compression equipment as they cost around INR 30-50 K. Routine Crepe bandages are used as part of compression therapy to reduce limb swelling and prevent recurrent infections The technique involves applying firm pressure, ideally as part of a, Multi-Layered Lymphedema Bandaging (MLLB) system. Key Principles of Crepe Bandage Application in India include i) The bandage should apply high pressure at the ankle and gradually decreasing pressure towards the knee or thigh (distal-to-proximal gradient) to push the lymph upwards ii) Crepe bandage is applied over a protective layer, such as cotton cloth or tube grip, to prevent skin direct contact and damage iii) Figure-of-eight or spiral techniques are commonly used iv) Starts from the foot (often covering toes individually with smaller bandages) and moves up to the knee or groin, depending on the swelling's extent v) The goal is firm, comfortable, and consistent pressure. It should not be so tight that it causes pain, numbness, or cyanosis (blue toes), but tight enough to support the limb vi) Bandages are typically worn while walking (ambulant) and removed at night or kept on for 24 hours except for daily cleaning/exercise routine [5].
Alternative/Supplementary Methods: In some Indian clinical settings, a "bandage boot" (crepe bandage applied over cotton and sometimes glued with dextrin) is used for severe cases, or multi-layer compression (using padding + crepe + cohesive bandage
Pneumatic pressure, specifically in the form of Intermittent Pneumatic Compression (IPC) or Sequential Intermittent Pneumatic Compression (SIPC): IPC and SIPC play a critical, evidence-based role in the conservative management of chronic lymphedema caused by filarial elephantiasis. It acts as an effective, non-invasive method to reduce limb volume and decrease the frequency of acute, severe infections (adenolymphangitis) [6].
The detailed role of pneumatic pressure in treating filarial elephantiasis include:
- Mechanism of Action: Pneumatic compression devices, often using multi-chambered sleeves (e.g., 12-cell instruments), apply air-powered, sequential pressure from distal to proximal (from toes/fingers up towards the torso).
- Fluid Mobilization: The pressure "milks" the accumulated, protein-rich oedematous fluid from the swollen, obstructed tissue back into functioning lymphatic vessels & circulation.
- Reduced Interstitial Pressure: increases tissue pressure, which forces fluid across the capillary bed into the venous system, reducing the overall volume.
- Increased Lymph Flow: SIPC accelerates lymphatic flow, helping to move fluid away from oedematous, obstructed regions.
Clinical Benefits: All the above mechanisms lead to Clinical Benefits of i) SIPC, in grades II and III filarial lymphedema, achieves a 20% to 60% reduction in limb circumference ii) Decreased Frequency of Infection (ADL): A major advantage is the reduction of Acute Dermatolymphangioadenitis (ADLA) attacks—the sudden, painful swelling caused by secondary bacterial infections and iii) Improved Mobility: By reducing the volume and hardness of the limb, it improves functionality and decreases cosmetic disfigurement.
Alternative to Manual Therapy: It provides a reliable alternative for patients who do not have access to trained therapists for Manual Lymphatic Drainage (MLD).
3. Application and Limitations:
Dosage and Duration: Typical sessions last 45-60 minutes, two to three times a day, though some studies suggest 2-3 hours daily for maximum effect.
Maintenance Required: The effects are not permanently sustained if the treatment is stopped. Long-term management requires a follow-up with compression garments or bandages to maintain the reduction.
Contraindications: It cannot be used in cases of active, severe infection (cellulitis), deep vein thrombosis, or uncontrolled heart failure.
Best Used in Combination: It is most effective as part of a comprehensive management program that includes skin care, elevation, and exercise [6].
4. Comparison to Other Methods
Manual Massage: While manual drainage is effective, pneumatic pumps can be used for longer durations and in rural, low-resource settings, serving as a more accessible alternative.
Surgical debridement: Pneumatic compression is a first-line non-operative therapy, whereas surgery is usually reserved for advanced, fibrotic cases [6].
A study on the use of sequential intermittent pneumatic compression (SIPC) in patients in which a 12-celled instrument capable of providing sequential compression from the distal to proximal direction was used in 28 patients with unilateral grades II (n=17) and III (n=11) filarial lymphoedema in a planned 4-week session. The patients were followed up for 6 months after compression therapy by water displacement volumetry. The results showed that 12 patients with grade II filarial lymphoedema had >26% reduction in oedema volume immediately after compression, but this reduction (>26%) was maintained in only 7 at 6 months. The corresponding figures for grade III cases were 6 & 4, respectively. The effect in grade III was less sustained than grade II. No complications attributable to SIPC were seen. An added advantage of SIPC was a significant decrease in attacks of adenolymphangitis after compression when compared to pre-compression frequency. These observations were seen even with non-compliance to both foot care measures and use of bandages to maintain reduction in oedema volume [6].
Morbidity Management and Disability Prevention (MMDP): The focus has shifted to managing existing lymphedema swollen limbs to prevent progression to elephantiasis [5,6].
Home-based management of lymphedema in India: Foot Hygiene is essential to prevent secondary infections (bacteria/fungi), focusing on washing, drying, and skin care ii) Use of proper footwear is encouraged to prevent injuries that trigger acute attacks iii) Active management involving limb exercises to improve lymph flow. Acute Attack Management: Addressing Acute Dermato-lymphangio-adenitis (ADLA) episodes through antibiotics, anti-inflammatory drugs to prevent further lymphatic damage. Vector Control: Continued use of conventional insecticides and, increasingly, environmental management to reduce vector breeding sites. Technological Advancements in Diagnosis: Increased use of rapid antigen tests (like Filaria test strips) for mapping and monitoring, which are more accurate than earlier methods.
Integrated Care: Integrating lymphedema management into the existing health system to improve access to care in rural and endemic urban localities [6].
Filarial Hydrocele: The most apparent symptom of a hydrocele is swelling in the scrotum, which is usually painless, but can be uncomfortable as the size increases over time. In some cases, a hydrocele may become infected, leading to additional symptoms such as redness, warmth, and increased pain. Filaria Hydrocele cases are seen in youngsters as young as aged 18 years and the oldest 76 years. Almost all cases have straw coloured hydrocele fluid, only a few may have milky fluid suggestive of chylocele. The average amount of fluid is about 500cc with a range from 200 to 1500cc. Surgery remains the mainstay of treatment, if a hydrocele does not resolve on its own after a few months, of medicinal treatment. In infants and children, surgery is recommended to prevent complications. The authors experience of doing vasectomies in mid-seventies (1972-75), puts the filarian hydrocoele rate at around 10% of cases who came for Vasectomy in Northern districts (now called Kalyan Karnataka) . Hydrocele surgeries in India have evolved from conventional, inpatient open surgeries to minimally invasive, outpatient, and laser-assisted techniques over the last century. While Jaboulay's and Lord's procedures are two common surgical techniques (hydrocelectomy) used to treat hydroceles in adults by addressing the tunica vaginalis sac.
Lord’s Procedure (Plication): Best for small to medium-sized, thin-walled hydroceles. It involves opening the sac and bunching (plicating) the redundant tunica vaginalis with sutures, without requiring extensive dissection or delivery of the testis. This technique is generally associated with a lower risk of hematoma and bleeding.
Jaboulay’s Procedure (Eversion): Preferred for larger, thicker-walled hydroceles. It involves opening the sac, excising excess tissue, and everting (turning inside out) the remaining tunica vaginalis behind the testis. It typically requires more extensive dissection than the Lord's procedure.
The indications of the surgery include i) a significantly large hydrocele causing discomfort interfering with daily activities ii) If a hydrocele becomes infected, leading to symptoms such as fever, redness, and increased pain surgery is done to drain the fluid & treat the infection iii) If imaging studies or physical examination raise concerns about the possibility of a tumour or other serious condition, hydrocele surgery is performed to obtain a definitive diagnosis and treat any underlying issues iv) In cases where a hydrocele has recurred after previous treatment, surgery may be the best option to prevent further recurrences. Since late 1990’s newer technique of i) Laparoscopic Hydrocelectomy, ii) Laser Hydrocelectomy & iii) Needle Aspiration with Sclerotherapy have evolved and are advocated. Laparoscopic Hydrocelectomy, a minimally invasive, keyhole technique results in less pain and faster recovery. Laser Hydrocelectomy uses laser technology to reduce bleeding, say and Drainage with a needle, with medication, is opted for patients unsuitable for surgery, known as Needle Aspiration with Sclerotherapy. Hydrocele surgery is not the subject of discussion of this article.
Burden of Lymphatic Elephantiasis in India: Indian States of Bihar, Jharkhand, Uttar Pradesh, Odisha, and Telangana, have highest burden. Other states of significant endemicity include Andhra Pradesh, Assam, Chhattisgarh, Gujarat, Karnataka, Kerala, Maharashtra, and West Bengal. Historically, Bihar has shown the highest endemicity (>17%), followed by Kerala (>15%) and Uttar Pradesh (>14%). In India Wuchereria Bancrofti is the dominant parasite (99.4% of cases), transmitted by Culex quinquefasciatus in urban and rural areas, while Brugia Malayi is restricted to specific rural areas in Kerala, Odisha, and others. In the home state of this author the Kalyan Karnatak districts of Bagalkot, Bidar, Vijayapura, Raichur Kalaburagi, and Udupi & Uttara Kannada in west coast in Karnataka are highly endemic for Filarial Hydroceles. India aims to eliminate Lymphatic Filariasis by 2027 through intensified MDA campaign [9.10]. Following the launch of a nationwide Mass Drug Administration (MDA) campaigns in February 2023, Karnataka’s focus is on selected pockets of Vijayapura, Bidar and Kalaburagi. Karnataka is one among the ten high-burden States in the country, with 12,000 chronic cases of LF in 2023 [11].
Government of India (GOI) - Ministry of Health & Family Welfare (MoH&FW) Response to the Problem: The GOI has recognized filarial lymphedema as a 'locomotor disability' under the Rights of Persons with Disabilities (RPwD) Act, 2016, allowing access to benefits for severely affected individuals.
The key milestones of Elimination of Lymphatic Filariasis in India are [10]:
- In 1997, The World Health Assembly adopted resolution WHA 50.29, for Elimination of Lymphatic Filariasis as a global public health problem by 2020.
- In 2002, National Health Policy set a goal for ELF in India by 2015, extended to 2017. It implied that LF ceases to be a public health problem when microfilaria rate is <1>
- In 2004, Elimination of Lymphatic Filariasis (ELF) programme was launched covering 202 endemic districts in 20 States/UTs.
- Subsequently scaled up to cover all the 257 endemic districts in 21 States/UTs targeting a population of about 650 million.
- In 2013 validation started through Transmission Assessment Survey (TAS).
- The policy decision to implement global strategy of co-administration of DEC with Albendazole during MDA was approved in 2006.
- Accelerated Plan for Elimination of Lymphatic Filariasis was launched in 10 Global Alliance Elimination of Lymphatic Filariasis (GAELF) on 13th June 2018.
- Triple Drug Therapy (IDA) trial started in 5 districts namely- Arwal (Bihar) and Simdega (Jharkhand), Nagpur (Maharashtra), Varanasi (Uttar Pradesh), Yadgiri (Karnataka) between 20th December and 13th November 2019.
- GOI has revised the financial norms for Morbidity Management Kits from Rs. 150/- to Rs. 500/- per kit in last MSG meeting held in February 2019.
Conclusion:
Lymphatic filariasis is a parasitic infection caused by 3 species of parasitic worms. In India it is mainly Wuchereria Bancrofti, transmitted by Culex. It causes chronic, irreversible lymphatic damage, leading to elephantiasis of legs or hydrocele of the scrotum. Lymphatic filariasis impairs the lymphatic system leading to an abnormal enlargement of body parts, causing pain, severe disability and social stigma. In India since 2023 the focus has shifted to managing existing lymphedema swollen limbs to prevent progression to elephantiasis which includes i) Home-based management of lymphedema following Foot Hygiene, to prevent secondary infections, ii) Use of proper footwear is encouraged to prevent injuries that trigger acute attacks iii) Active management involving limb exercises to improve lymph flow iv) Addressing Acute Dermato-lymphangio-adenitis (ADLA) episodes through antibiotics, anti-inflammatory drugs v) Continued use of conventional insecticides for vector control and, reducing vector breeding sites vi) Increased use of rapid antigen tests for mapping and monitoring and vii) Integrating lymphedema management into the existing health system to improve access to care in rural and endemic urban localities. viii) Promoting Crepe Bandage & Pneumatic compressors use for individual case management.
References
- World Health Organization, (2024). Lymphatic filariasis: Key facts, WHO Website.
View at Publisher | View at Google Scholar - Das LK et al., (2008). Locomotor disability in bancroftian filarial lymphoedema patients, Communicable Diseases, 40(1), 13–19.
View at Publisher | View at Google Scholar - Indian Journal of Plastic Surgery, (2024). Filarial elephantiasis of lower extremity: A review, 18(1), 22–34.
View at Publisher | View at Google Scholar - ResearchGate, (2024). Filarial elephantiasis of lower extremity: A review, Online Source.
View at Publisher | View at Google Scholar - Gogia et al., (2025). Lymphedema management in a filaria endemic area, Indian Journal of Surgery, 87(2), 411–412.
View at Publisher | View at Google Scholar - Manjula Y et al., (2002). Evaluation of sequential intermittent pneumatic compression for filarial lymphoedema, National Medical Journal of India, 15(4), 192–194.
View at Publisher | View at Google Scholar - Savita KS, (2014). Hydrocele management in a filaria endemic area, Indian Journal of Basic and Applied Medical Research, 4(1), 447–450.
View at Publisher | View at Google Scholar - Galani P et al., (2015). Hydrocele management in a filaria endemic area, Journal of Advanced Medical and Dental Sciences Research, 3(5), S17–S19.
View at Publisher | View at Google Scholar - National Center for Vector Borne Diseases Control, (2024). Revised guideline on elimination of lymphatic filariasis, Government Report.
View at Publisher | View at Google Scholar - National Center for Vector Borne Diseases Control, (2026). Elimination of lymphatic filariasis in India, Government Report.
View at Publisher | View at Google Scholar - The Hindu, (2023). Elimination of lymphatic filariasis: Karnataka starts mass drug administration in three high-transmission districts, Newspaper Article.
View at Publisher | View at Google Scholar

 Clinic
Clinic
