Research Article | DOI: https://doi.org/10.31579/ 2834-8419/005
Surgical Site Infection: Impacts and Challenges of Antibiotic Rationalism
- Chowdhury *
- Navim Kabir
Emergency Medical Officer, Islami Bank Central Hospital, Kakrail, Dhaka, Bangladesh.
*Corresponding Author: Chowdhury, Emergency Medical Officer, Islami Bank Central Hospital, Kakrail, Dhaka, Bangladesh
Citation: Chowdhury, Navim Kabir. (2022). Surgical Site Infection: Impacts and Challenges of Antibiotic Rationalism. Clinics In Radiology. 1(1); DOI:10.31579/ 2834-8419/005
Copyright: © 2022 Chowdhury, Kabir N., This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 06 October 2022 | Accepted: 10 October 2022 | Published: 21 October 2022
Keywords: nosocomial; contaminated; mrsa; who; antimicrobial resistance
Abstract
Surgical site infection (SSI) is one of the most common hospital acquired infections, and according to recent studies its incidence is estimated to approximate 10% for all surgical interventions . SSIs are associated with increased antimicrobials resistance, treatment costs, prolonged hospital stay and increased mortality. They can also cause disfiguring scars, which can be problematic, particularly for young adults. Comorbidities along with inappropriate debridement procedure, unhealthy hospital environment, habitual activity, immune suppression, nutritional deficiency, hypersensitivity causes prolong would healing. Here the scenario of post operative surgical site infection with challenges and management has been highlighted in 107 patients who come in emergency department in post surgical procedure dressing purpose and those who admit in indoor patient department after operative procedure.
1. Introduction
Surgical procedures are one of the most sensitive and vital part of treatment management. Different diseases which are not enough responsive to conservative treatment due to bad prognosis. For patient’s life safety and proper treatment surgeons take the responsibility upon their shoulder. Though surgical procedure for the sake of patient’s purpose, in some cases postoperative infection specially in surgical site becomes a burning issue for patient’s management. Nosocomial infection along with other factors create the barrier in the management.
1. Introduction
Surgical procedures are one of the most sensitive and vital part of treatment management. Different diseases which are not enough responsive to conservative treatment due to bad prognosis. For patient’s life safety and proper treatment surgeons take the responsibility upon their shoulder. Though surgical procedure for the sake of patient’s purpose, in some cases postoperative infection specially in surgical site becomes a burning issue for patient’s management. Nosocomial infection along with other factors create the barrier in the management.
2.Classification of Surgical Wound
According to Centre for Disease Control and Prevention (CDC) surgical wound classified into following group:
Class I/ Clean: No evidence of infection and inflammation may be found. Respiratory, genital, alimentary tracts are not involved. Primary closure is applicable and according to the need drain tube may be inserted. If blunt trauma is not followed, opearative incisional wound may be included after meeting the criteria. [1] [2]


Class II/Clean-Contaminated: Here respiratory, genital, urinary tract may be involved and contamination is unusual. Billiary tract, oropharynx, vagina, appendix are involved where no evidence of infection or breach of sterility is found [3] .
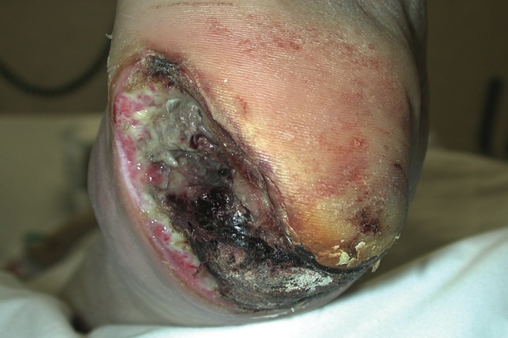
Class III/Contaminated: Open, fresh wound where breach of sterility occurs with gross spillage from Gastro Intestinal tract ( GIT).No evidence of purulent discharge is found. [4][5]

Class IV/ Dirty wound: Presence of devitalized tissue that is involved with clinical infection and visceral perforation. Existence of infection can be found in operation table before operation. [6]
3.Prevalance
This manuscript, the skin infection of the patients who come to the emergency department for dressing purpose and indoor patients wound condition after surgery has been highlighted.60 patients who come towards emergency department for wound dressing purpose who willingly participate to study with their health related info. [7] [8] Besides 47 patients from indoor (having postoperative status) participated. They are asked about their comorbidities, lifestyle, habitual activity, dietary habit, drug history, previous operative history. [9,10,11]
In emergency patients about 60% wound are clean cut types due to RTA or other mechanical injury. About 80% were male and 20% were female. Some were wounded due to physical assault. Female were predominant in physical assault.In some cases due to fearness or unawareness they did not come towards the hospital. That made clean wound to contaminated, in some cases dirty. 10
4.Result
Above discussion we see that postoperative surgical site infection and its management depends mostly on co morbidities and nosocomial infection. Nosocomial infection predominantly on indoor patient due to prolonged operative process, in situ instruments and different invasive procedure. Staphylococci are predominant in organisms and specially for gram positive and E.coli in gram negative. We follow culture sensitivity for detecting the organism as well as proper anti microbial compound.
5.Discussion
According to history and observation etiologies, management have been correlated for treatment purpose.
5.Discussion
According to history and observation etiologies, management have been correlated for treatment purpose.
6.Etiologies
Surgical risk factors include prolonged procedures and inadequacies in either the surgical scrub or the antiseptic preparation of the skin. Physiological states that increase the risk of SSI include
- Trauma
- Shock
- Blood transfusion
- Hypothermia
- Hypoxia
- Hyperglycemia.
But Nosocomial Infection associated irrational uses of antibiotics results antimicrobial resistance which becomes significant traits for SSI. [32-34]
7.Mechanism of Antimicrobial Resistance
Activation of antimicrobial resistance induced by 4 methods:
- Limiting uptake of a drug
- Modifying a drug target
- Inactivation of a drug
- Active drug efflux.
Intrinsic resistance activate drug resistance all 4 except target site modification of a drug procedure. Due to structural differences activation process of drug resistance between gram positive and gram negative bacteria is different. Gram negative bacteria use above 4 mechanisms whereas gram positive bacteria hardly follow limiting uptake due to absence of Lipopolysaccharide ( LPS) in cell membrane. Besides gram positives haven’t specific mechanism for drug efflux process. [33-36]
8.Management of Anti Microbial Resistance (ABR)
The World Health Organization (WHO) endorsed a global action plan to tackle antimicrobial resistance. It sets out five strategic objectives:
Improving awareness and understanding of antimicrobial resistance.
To strengthen knowledge through surveillance and research.
Reducing the incidence of infection
Optimal the use of antimicrobial agents; and
Developing the economic case for sustainable investment that takes account of the needs of all countries, and increase investment in new medicines, diagnostic tools, vaccines and other interventions. [37]
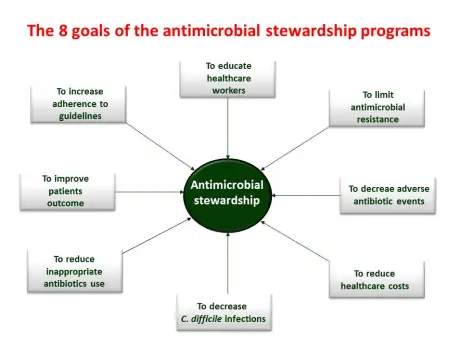
Antimicrobial application is a vital point to manage surgical site infection management. Specially in a country like Bangladesh some additional preventive measures that can be great advantage to protect human life. Like-
- Create awareness about post/post procedural dressing. Proper wound debridement be a dynamic step for reducing recovery time.
- Antibiotic should not be sold without registered physician’s written prescription. People unawefully buy antibiotics and it was about 15-20% that we know during taking drug history from the patients.
- In grass root level people are not enough solvent to buy costly drugs specially oral/ injectable antibiotics. Pharmaceuticals company should think how can improve and increase production process with thinking generalized cost effectiveness.
- Biotechnology sector should be emphasized.
- Governmental/ Non governmental logistics support should be widen for expanding pharma sector.
- Laboratory facilities like CBC, blood culture and other microbiological investigations should be practiced rationally. Cost effectiveness should be in priority basis. [38-39]
9. Conclusion
Undoubtedly post operative management is an important traits for preventing infection. Lack of awareness, body mechanism and others associated circumstancial factors make it aggressive and turns to septicemia in advanced cases. Pharmacological specially antibiotic is an achievement rather it become resistant due to proper monitoring and irrational use. Making the goal of antibiotic extraordinary for the people, nonpharmacological actions, research could be more effective and make effective management protocol to form healthy infection free earth.
10. Acknowledgement
Dr Nurul Islam MBBS,DLO Emergency Medical Officer, Islami Bank Central Hospital,Kakrail, Dhaka, Bangladesh.
11. Funding Information
No funding assistance applicable to this manuscript.
12. Competing Interest
The author have no competing interests to declare.
References
- Rahman MS, Hasan K, Ul Banna H, Raza AM, Habibullah T. (2019). A study on initial outcome of selective non-operative management in penetrating abdominal injury in a tertiary care hospital in Bangladesh. Turk J Surg. 35(2):117-123.
View at Publisher | View at Google Scholar - Young PY, Khadaroo RG. (2014). Surgical site infections. Surg Clin North Am. 94(6):1245-1264.
View at Publisher | View at Google Scholar - Vitiello R, Perna A, Peruzzi M, Pitocco D, Marco G. (2020). Clinical evaluation of tibiocalcaneal arthrodesis with retrograde intramedullary nail fixation in diabetic patients. Acta Orthop Traumatol Turc. 54(3):255-261.
View at Publisher | View at Google Scholar - Spagnolo AM, Ottria G, Amicizia D, Perdelli F, Cristina ML. (2013). Operating theatre quality and prevention of surgical site infections. J Prev Med Hyg. 54(3):131-137.
View at Publisher | View at Google Scholar - Kamel C, McGahan L, Mierzwinski-Urban M, Embil J. (2011). Preoperative Skin Antiseptic Preparations and Application Techniques for Preventing Surgical Site Infections: A Systematic Review of the Clinical Evidence and Guidelines [Internet]. Canadian Agency for Drugs and Technologies in Health.
View at Publisher | View at Google Scholar - Culver DH, Horan TC, Gaynes RP, Martone WJ, Jarvis WR, et al. (1991). Surgical wound infection rates by wound class, operative procedure, and patient risk index. National Nosocomial Infections Surveillance System. Am J Med. 91(3B):152S-157S.
View at Publisher | View at Google Scholar - López Pereira P, Díaz-Agero Pérez C, López Fresneña N, Las Heras Mosteiro J, Palancar Cabrera A, et al. (2017). 'Epidemiology of surgical site infection in a neurosurgery department'. Br J Neurosurg. 31(1):10-15.
View at Publisher | View at Google Scholar - Owens CD, Stoessel K. (2008). Surgical site infections: epidemiology, microbiology and prevention. J Hosp Infect. 70 Suppl 2:3-10.
View at Publisher | View at Google Scholar - Sanger PC, Simianu VV, Gaskill CE, Armstrong CA, Hartzler AL, et al. (2017). Diagnosing Surgical Site Infection Using Wound Photography: A Scenario-Based Study. J Am Coll Surg. 224(1):8-15.
View at Publisher | View at Google Scholar - van Walraven C, Musselman R. (2013). The Surgical Site Infection Risk Score (SSIRS): A Model to Predict the Risk of Surgical Site Infections. PLoS One. 8(6): e67167.
View at Publisher | View at Google Scholar - Bustamante-Munguira J, Herrera-Gómez F, Ruiz-Álvarez M, Figuerola-Tejerina A, Hernández-Aceituno A. (2019). A New Surgical Site Infection Risk Score: Infection Risk Index in Cardiac Surgery. J Clin Med. 8(4).
View at Publisher | View at Google Scholar - Emori TG, Culver DH, Horan TC, Jarvis WR, White JW. (1991). National nosocomial infections surveillance system (NNIS): description of surveillance methods. Am J Infect Control. 1991 Feb;19(1):19-35.
View at Publisher | View at Google Scholar - Figuerola-Tejerina A, Bustamante E, Tamayo E, Mestres CA, Bustamante-Munguira J. (2017). Ability to predict the development of surgical site infection in cardiac surgery using the Australian Clinical Risk Index versus the National Nosocomial Infections Surveillance-derived Risk Index. Eur J Clin Microbiol Infect Dis. 36(6):1041-1046.
View at Publisher | View at Google Scholar - Berríos-Torres SI, Umscheid CA, Bratzler DW, Leas B, et al. (2017). Centers for Disease Control and Prevention Guideline for the Prevention of Surgical Site Infection, 2017. JAMA Surg. 152(8):784-791.
View at Publisher | View at Google Scholar - Lall RR, Wong AP, Lall RR, Lawton CD, Smith ZA, et al. (2015). Evidence-based management of deep wound infection after spinal instrumentation. J Clin Neurosci. 22(2):238-242.
View at Publisher | View at Google Scholar - Yin D, Liu B, Chang Y, Gu H, Zheng X. (2018). Management of late-onset deep surgical site infection after instrumented spinal surgery. BMC Surg. 18(1):121.
View at Publisher | View at Google Scholar - Franklin S, Sabharwal S, Hettiaratchy S, Reilly P. (2020). When infection isn't infection. Ann R Coll Surg Engl. 102(8): e183-e184.
View at Publisher | View at Google Scholar - Sagawa M, Yokomizo H, Yoshimatsu K, Yano Y, Okayama S, et al. (2017). [Relationship between Surgical Site Infection (SSI) Incidence and Prognosis in Colorectal Cancer Surgery]. Gan To Kagaku Ryoho. 44(10):921-923.
View at Publisher | View at Google Scholar - Isik O, Kaya E, Dundar HZ, Sarkut P. (2015). Surgical Site Infection: Re-assessment of the Risk Factors. Chirurgia (Bucur). 110(5):457-461.
View at Publisher | View at Google Scholar - Breithaupt T. (2010). Postoperative glycemic control in cardiac surgery patients. Proc (Bayl Univ Med Cent). 23(1):79-82.
View at Publisher | View at Google Scholar - Epstein NE. (2018). Preoperative measures to prevent/minimize risk of surgical site infection in spinal surgery. Surg Neurol Int. 9:251.
View at Publisher | View at Google Scholar - Poggio JL. (2013). Perioperative strategies to prevent surgical-site infection. Clin Colon Rectal Surg. 26(3):168-173.
View at Publisher | View at Google Scholar - Anderson PA, Savage JW, Vaccaro AR, Radcliff K, Arnold PM, et al. (2017). Prevention of Surgical Site Infection in Spine Surgery. Neurosurgery. 80(3S): S114-S123.
View at Publisher | View at Google Scholar - Barie PS, Eachempati SR. (2005). Surgical site infections. Perioper Issues Surg. 85(6): 1115–1135.
View at Publisher | View at Google Scholar - Berríos-Torres SI, Umscheid CA, Bratzler DW, et al. (2017). Centers for Disease Control and Prevention guideline for the prevention of surgical site infection, 2017. JAMA Surg. 152(8): 784–791.
View at Publisher | View at Google Scholar - Levine NS, Lindberg RB, Mason ADJ, Pruitt BAJ. (1976). The quantitative swab culture and smear: A quick, simple method for determining the number of viable aerobic bacteria on open wounds. J Trauma. 16(2): 89–94.
View at Publisher | View at Google Scholar - Satzke C, Seduadua A, Chandra R, Carapetis JR, Mulholland EK, et al. (2010). Comparison of citrated human blood, citrated sheep blood, and defibrinated sheep blood Mueller-Hinton agar preparations for antimicrobial susceptibility testing of Streptococcus pneumoniae Isolates. J Clin Microbiol. 48(10): 3770.
View at Publisher | View at Google Scholar - Lai PS, Bebell LM, Meney C, Valeri L, White MC. (2017). Epidemiology of antibiotic-resistant wound infections from six countries in Africa. BMJ Glob Health. 2017; 2(Suppl 4): e000475.
View at Publisher | View at Google Scholar - Kawakita T, Landy HJ. (2017). Surgical site infections after cesarean delivery: Epidemiology, prevention and treatment. Matern Health Neonatol Perinatol. 3: 12.
View at Publisher | View at Google Scholar - Becker K, Heilmann C, Peters G. (2014). Coagulase-negative staphylococci. Clin Microbiol Rev. 27(4): 870–926.
View at Publisher | View at Google Scholar - Kloos WE, Bannerman TL. (1994). Update on clinical significance of coagulase-negative staphylococci. Clin Microbiol Rev. 7(1): 117–140.
View at Publisher | View at Google Scholar - Asim P, Naik NA, Muralidhar V, Vandana KE, Varsha AP. (2016). Clinical and economic outcomes of Acinetobacter vis a vis non-Acinetobacter infections in an Indian teaching hospital. Perspect Clin Res. 7(1): 28–31.
View at Publisher | View at Google Scholar - Lee N-Y, Lee H-C, Ko N-Y, et al. (2007). Clinical and economic impact of multidrug resistance in nosocomial Acinetobacter baumannii bacteremia. Infect Control Hosp Epidemiol. 28(6): 713–719.
View at Publisher | View at Google Scholar - Onken A, Said AK, Jørstad M, Jenum PA, Blomberg B. (2015). Prevalence and antimicrobial resistance of microbes causing bloodstream infections in Unguja, Zanzibar. PloS One. 10(12): e0145632.
View at Publisher | View at Google Scholar - Allegranzi B, Bagheri Nejad S, Combescure C, et al. (2011). Burden of endemic health-care-associated infection in developing countries: Systematic review and meta-analysis. Lancet Lond Engl. 377(9761): 228–241.
View at Publisher | View at Google Scholar - Lowings M, Ehlers MM, Dreyer AW, Kock MM. (2015). High prevalence of oxacillinases in clinical multidrug-resistant Acinetobacter baumannii isolates from the Tshwane region, South Africa–an update. BMC Infect Dis. 15: 521.
View at Publisher | View at Google Scholar - Lob SH, Hoban DJ, Sahm DF, Badal RE. (2016). Regional differences and trends in antimicrobial susceptibility of Acinetobacter baumannii. Int J Antimicrob Agents. 47(4): 317–323.
View at Publisher | View at Google Scholar - Hadjisymeou S, Loizou P, Kothari P. (2013). Lactococcus lactis cremoris infection: Not rare anymore? BMJ Case Rep. bcr2012008479.
View at Publisher | View at Google Scholar - Kallstrom G. (2014). Are quantitative bacterial wound cultures useful? J Clin Microbiol. 52(8): 2753–2756.
View at Publisher | View at Google Scholar

 Clinic
Clinic